
Lymphoma treatment in Israel
- An excellent result is guaranteed by doctors we have carefully selected over 9 years
- Full trip organization and doctor’s support 7 days a week


You don't pay for the services of Experts Medical
as we are representatives of more than 100 foreign clinics

You get treatment without extra fees
You make all payments only at the clinic upon arrival
The best doctors
Professor Dina Ben-Yeguda is Israel’s leading hematologist oncologist, director of Hadassah’s hematology department, founder of the laboratory for molecular diagnostics of hematological diseases and fundamental research.
Specialization:
- Molecular diagnosis of hematological diseases
- Malignant blood diseases
- Bone marrow transplantation
- Gene therapy
- Immunology
Awards:
- In 2017, Professor Ben Yehuda became the 23rd dean of the Hadassah School of Medicine and the first woman to lead the medical school in its more than 70-year history.
- Professor Dina Ben-Yehuda became the first female military member to receive the Chief of Staff Award for her initiative in collecting information about those killed or missing in action.
- Recently, Dina Ben-Yehuda was awarded the prize of the foundation named after Daniel Sonnenfeld “Healing with the Heart”. The honorary award is given to doctors and nurses who go beyond the scope of their profession and do much more for patients than dictated by medical ethics.
Membership in professional communities:
- Israel Society of Hematologists
- International Society of Hematologists
- Israel Society of Hemato-Oncology
- International Society of Hemato-oncology
Doctor of Medical Sciences.
Specialization: hematology.
Graduated from the Medical Faculty of the Hebrew University with a degree in Medicine
Advanced Training at Tel Aviv Medical Center
Among the best oncohematologists in Israel according to Forbes in 2021, 2022, 2023.
Professor Avivi graduated with honors from the medical faculty of Teknon. She specialized in the treatment of lymphoma and myeloma.
Since 2014, she has been working as the head of the hematology department at the Tel Aviv Medical Center. In addition to her work at the hospital, Professor Avivi works as the head of the Department of Hematology at Tel Aviv University.
Professor Avivi conducts clinical and laboratory research related to various hematological malignancies and develops methods to activate the immune system against malignant cells. As part of these studies, she led a joint program with Harvard University in which myeloma patients were treated with personalized vaccines composed of dendritic cells combined with disease cells.
Prof. Avivi is actively involved in a variety of medical projects and research in Israel and around the world, including innovative drugs and treatment approaches. She is also a member of several working groups, including the European Group on Hematological Malignancies in Pregnancy and the European Mantle Cell Lymphoma Group.
Director of the Myeloma Department of the Tel Aviv Sourasky Medical Center (Ichilov Hospital) and Head of the Israel Myeloma Department
Main area: hematology, internal medicine
Secondary field: multiple myeloma
Clinical Associate Professor at the Sackler School of Medicine, actively teaching physicians, medical students, and research students. She leads, initiates and participates in various medical research in the field of myeloma in Israel and around the world, principal investigator in the development of drugs for myeloma.
Prof. Cohen is the co-author of 90 articles and papers. Serves as a medical advisor to the AMAN Association (Association of Myeloma Patients in Israel) and is a member of the Higher Committee of the Ministry of Health for Clinical Research.
The best clinics for Lymphoma treatment in Israel


















we will contact you within 15 minutes
Lymphoma treatment programs in Israel
High-dose chemotherapy with bone marrow transplant
- Hospitalization: 90 days
- Duration of stay in Israel: 90 days
- Payment assistance from Experts Medical: up to 11 000 USD (PATIENTS UNDER 18)
- Days 1-4: Examination
- Day 5: Collection of own stem cells
- Day 6: High dose chemotherapy
- Day 7: Autologous bone marrow transplant
- Day 47: Discharge from the hospital and accommodation in a hotel with weekly control tests
- Day 90: Return home
Chemotherapy for Lymphoma treatment in Israel
- Hospitalization: 30 days
- Payment assistance from Experts Medical: up to 11 000 USD (PATIENTS UNDER 18)
- Day 1: Meeting at the airport, consultation, examination
- Day 5: Hospitalization
- Day 35: Check-out, hotel check-in
Treatment of Lymphoma in Israel is one of the most sought-after medical areas among foreign patients. This is due to the prevalence of the disease in different ethnic groups and age categories. According to the American Organization for Cancer Statistics, lymphomas are among the ten most common cancers among men and women.
What is lymphoma and what types of it exist?
Lymphoma is a common term for cancer that develops in the lymphatic system. Cancer cells attack tissues and organs that produce and transport infection-fighting white blood cells.

Oncologists distinguish two main types of this tumor, depending on the type and degree of malignancy of the cells:
– Hodgkin’s lymphoma (lymphogranulomatosis), which spreads through the lymphatic system in a relatively orderly way and responds well to treatment;
– non-Hodgkin’s lymphoma (NHL), a large group of diseases ranging from relatively benign, sluggish to extremely malignant and aggressive.
Follicular lymphoma is the most frequently diagnosed of the first subgroup, while diffuse B-cell lymphoma is the most frequently diagnosed of the second.
What are the causes of lymphoma?
The most common causes of lymphoma include:
- drugs that suppress the immune system (immunosuppressants);
- contact with chemicals;
- abnormal increase in the production of lymphocytes (lymphocytosis);
- genetic mutations (eg, SOCS1 is found in B-cell and follicular lymphoma).
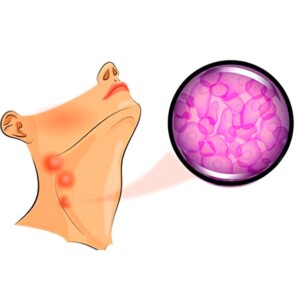
The disease was first described in 1832 by an English scientist, Sir Thomas Hodgkin. This is where lymphoma gets its name. Lymphogranulomatosis (the second name of this disease) is a malignant neoplasm, in which giant tumor elements are found in the lymph nodes – Berezovsky-Sternberg-Reed cells. More often, the cervical or supraclavicular lymph nodes become the source.
Given the long history of the disease, the world’s leading scientists are focused on fighting this type of cancer. Israeli oncologists have long been part of a large coalition of specialists who test new methods of lymphoma therapy for patients of different ages. For the treatment of lymphoma in Israel for the period of 2023, more than 200 clinical trials of new anti-cancer drugs are being conducted.
Foreign patients prefer the treatment of lymphomas in Israeli clinics mainly for two reasons. One of them is the inaccessibility of modern and safe drugs and methods that can cure cancer. Another reason is the high cost of certain types of procedures in countries with developed medicine. Therefore, the price for the treatment of lymphoma in Israel will be 20-30% less, which is the “golden mean” in the matter of choosing where the patient can cure the disease.
What is interesting to know about the treatment of lymphoma in Israel?

According to Israeli multidisciplinary clinics, up to 90% of children and 70% of adult patients achieve complete remission of lymphoma within 3 months thanks to CAR-T gene therapy. Gene therapy is also widely used at Sheba Hospital in Tel Aviv.
In many countries, targeted and immune therapies may be available to patients. But often in clinics in Asia and Eastern Europe, these treatments are carried out on the basis of the availability of drugs without any individual testing for the sensitivity of cancer to them. For the treatment of lymphoma in Israel, special tests are carried out that allow to accurately select drugs. FoundationOne Heme is a study that identifies genomic changes in the DNA and RNA of cancer patients. This unique diagnostics is available only in advanced medical centers.
Thanks to the FoundationOne Heme test, Israeli oncologists select an effective targeted or immune drug for each patient with lymphoma. At Hadassah Hospital in Jerusalem, this research method is available. It is also performed for leukemia (a malignant disease of the hematopoietic system) and myeloma (plasma cell cancer).
The success of lymphoma treatment in Israel is due to modern medical technologies that doctors use for diagnosis. Reliable oncological check-ups are available to residents and guests of the country, which allow to detect the disease at an early stage. If a person has already been sick for some time, then he will be able to undergo a comprehensive examination to clarify all the details of the disease with further selection of effective drugs against lymphoma.

In addition, some of the biopsy samples will be used for other tests to confirm the diagnosis and more accurately identify the specific lymphoma subtype. This approach allows doctors in Israel to determine the most effective treatment tactics for the patient.
At each stage of the examination, the doctor receives all the necessary data for making a diagnosis: the stage of the lymphoma, the prevalence of the oncological process in the body, and the state of other organs and body systems against the background of cancer. The sequence of procedures may differ in different Israeli hospitals but the principles of research and the benefits of them remain unchanged.
Typically, diagnosis includes the following procedures:
- Biopsy
Depending on the medical condition, doctors may perform a biopsy in a variety of ways.
A bone marrow aspiration biopsy is the second most important diagnostic procedure. It is necessary to examine the cellular composition of the bone marrow to determine whether it is affected by tumorigenesis. The larger the sample, the more tissue the pathologist can examine, which increases the accuracy of the diagnosis.
During this procedure, the surgeon makes an incision to remove the entire lymph node (excisional biopsy) or most of the tissue (incisional biopsy).
If the lymph node is located close to the surface of the skin, the procedure can be performed under local anesthesia to numb the area. If the lymph node is in the chest or abdomen, the patient is sedated and the surgeon removes the tissue either laparoscopically (through a tube inserted into the abdomen) or through abdominal surgery.
Needle biopsy
This procedure is used when the lymph nodes are located deep in the chest, abdomen, or in other places that are difficult to access for the excisional tissue sampling method. In some cases, there may be medical reasons to avoid excisional or incisional biopsy.
During this procedure, a special needle is inserted into a lymph node having cancer, and a small sample of tissue is removed. The needle biopsy of the lymph node can be performed under local anesthesia.
Bone marrow aspiration
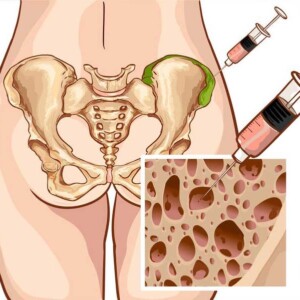
Bone marrow biopsy with aspiration is not used for initial diagnosis. An aspiration biopsy is needed to collect bone marrow for analysis before a stem cell transplant or for chromosome analysis. Bone marrow is a spongy, soft substance found inside bones where normal blood cells form.
During the aspiration part of this procedure, the doctor cleans and anesthetizes the skin over the thigh and inserts a thin, hollow needle into the bone. The doctor uses a syringe to remove a small amount of fluid from the bone marrow. Next, a biopsy is performed. The doctor inserts a slightly larger needle to take a small sample of bone and bone marrow.
Fine needle aspiration biopsy (FNA)
FAB is a biopsy performed with a thin needle. Due to the small diameter of the needle, the sample will only contain scattered cells from the lymph node.
A fine-needle biopsy is most often used to check for a return of the disease (relapse) and is almost never used for the initial diagnosis of lymphoma.
Lumbar puncture (cerebro-spinal tap)
Sometimes a lumbar puncture is used to determine if the lymphoma has spread to the cerebrospinal fluid. Most types of lymphoma do not spread to it. A doctor will only prescribe this test for patients with certain types of lymphoma or who have symptoms that indicate the cancer has spread to the brain.
For this procedure, the doctor inserts a thin needle into the lower back after this area has been set under local anesthesia. The doctor then uses a small needle to take a sample of the fluid, which will be sent to a lab for analysis.
A lumbar puncture can also be used to inject a small amount of chemotherapy directly into an area where cerebrospinal fluid circulates.
Collection of pleural or peritoneal fluid
This procedure is used to find out if the lymphoma has spread to the chest or abdomen, where it can cause fluid to build up.
For this procedure, the doctor sets the skin under local anesthesia, inserts a small needle, and uses a syringe to remove a sample of fluid for laboratory analysis. The fluid is called pleural if it is inside the chest, and peritoneal if it is inside the abdomen.
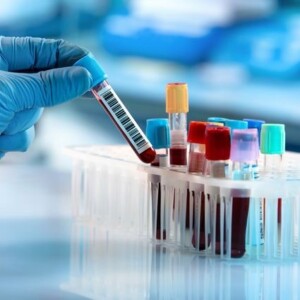
- Blood tests
Doctors take a patient’s blood for tests to measure the number of different types of cells – red blood cells, lymphocytes, white blood cells, and platelets. This information helps determine how advanced the lymphoma is and whether the patient will be able to tolerate certain treatments.
- Visual tests
The oncologist needs the results of imaging tests to find areas of the body where cancer may develop, to find out how widely metastases have spread. In the process of treatment, this is how they check how well the therapy works, which allows to make timely adjustments. Most of these tests are painless and do not require anesthesia.
In Israel, these hardware studies are carried out for lymphoma:
X-rays
When realizing X-rays, radiation to take pictures of areas inside the body is used. The dose of radiation used in most diagnostic tests is so low that it poses no risk to the patient. Findings on a chest X-ray can indicate whether the disease is invasive (large tumors or lymph nodes are usually resistant to conventional therapy).
Computed tomography (CT scan)
A CT scan takes X-rays of the body from different angles. The computer combines images taken from different angles to get a detailed picture of the organs inside the body. Patients with lymphoma often have CT scans of the neck, chest, abdomen, and pelvis. This shows how many lymph nodes are affected, how large they are, and whether the internal organs are damaged by the cancer.
Before the CT scan, the patient may be asked to drink contrast fluid or receive an intravenous injection of a contrast agent. This will give a clearer visualization of the anomalous areas.
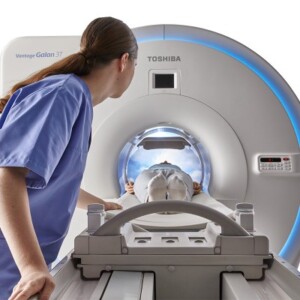
Magnetic resonance imaging (MRI)
Like a CT scan, an MRI takes images of the body from different angles. But an MRI machine doesn’t produce X-rays like a CT scan. Instead, it uses magnetic and radio frequency waves.
MRI can provide important information about tissues and organs, especially the nervous system, that cannot be obtained with other imaging modalities. Because this testing method works well for clear images of the bones, brain, and spinal cord, an MRI may be prescribed if the doctor wants to see if the lymphoma has spread to these areas. Diagnosis of lymphoma in Israel is carried out using the 3-Tesla MRI unit, which can detect even the smallest metastases up to 2 mm.
Positron emission tomography (PET scan)
For PET, radioactive fluorodeoxyglucose (a type of sugar) is first injected into the body. A positron camera is then used to detect radioactivity and take cross-sectional images of the body.
PET scan helps determine the extent to which the disease is present and how well the lymphoma is responding to treatment. While a CT scan shows the size of a lymph node, a PET scan shows activity. Israeli doctors conduct tests on a modern device of combined CT and PET systems, which is called PET-CT. Accurate diagnosis on PET-CT allows regular and demonstrative examinations to be carried out without harm to the patient’s body.
Multi-Gated Acquisition (MUGA Scan)
MUGA scan is an imaging test that assesses how well the heart muscle works. MUGA is done to test whether a patient’s body can withstand treatment with certain anti-lymphoma drugs, which in rare cases can damage the heart. Multi-Gated Acquisition can be performed even when patients are resting.
A two-dimensional echocardiogram (ECHO) is sometimes used instead of the MUGA scan to check heart function.
Function tests of lung
Lung function tests are done to assess whether a patient can tolerate certain types of lymphoma therapies that can interfere with bronchopulmonary function.
The tests before starting treatment are prescribed by the doctor. Also, lung function tests are carried out during therapy to assess the functioning of the organ.
Lymphoma treatment in Israel includes:
- Active Monitoring. Some forms of lymphoma grow slowly. In this case, the patient and the doctor can decide when to start therapy. From time to time, you can take tests to monitor the condition of the body.
- Chemotherapy. These are special drugs for the destruction of fast-growing cancer cells. The drugs are usually given through a vein, but they can also be taken as tablets, depending on the specific type of medication.
- Radiation therapy. In Israeli clinics, powerful linear accelerators are used. Directed beams of energy, such as X-rays and protons, destroy cancer cells. At the same time, there is practically no effect on healthy tissues. Therefore, after such radiation therapy, the patient will feel comfortable.
- Bone marrow transplantation. Bone marrow transplantation (BMT) involves the prior use of high doses of chemotherapy and radiotherapy to suppress the affected bone marrow. This is followed by the BMT of healthy stem cells from the patient or from a donor.
Other innovative methods used to treat lymphoma in Israel include targeted drugs that target specific abnormalities in cancer cells. Immunotherapy drugs use the patient’s own immune system to destroy the lymphoma. A specialized treatment is also referred to as CAR-T chimeric antigen receptor therapy. In this case, T-lymphocytes are involved, in fighting microbes. CAR-T therapy combines the possibilities of cellular, immunotherapy, and gene therapy for lymphoma.
 Targeted therapy for lymphoma is a type of treatment that uses drugs to target and target specific cancer cells. Targeted therapy (monoclonal antibodies) usually causes less damage to normal cells than chemotherapy or radiation therapy.
Targeted therapy for lymphoma is a type of treatment that uses drugs to target and target specific cancer cells. Targeted therapy (monoclonal antibodies) usually causes less damage to normal cells than chemotherapy or radiation therapy.
Monoclonal antibodies are immune system proteins developed in the laboratory to treat many complex diseases, including cancer. As a treatment for oncology, these antibodies can be attached to a target on atypical cells. Antibodies are able to destroy cancer cells, block growth and prevent their spread. Monoclonal antibodies are administered by infusion (into the bloodstream). They can be used alone or to deliver drugs, toxins, or radioactive material directly to a lesion. This method is often used to treat Hodgkin’s lymphoma.
Immune therapy is a treatment, in which the patient’s immune system is used to target cancer. Substances produced by the body or in a laboratory are used to enhance, direct, or restore the body’s natural defenses. Immunotherapy is a type of biological treatment for lymphoma.
How does immunotherapy work? PD-1 and PD-L1 inhibitor therapy. PD-1 is a protein on the surface of T cells that helps control the body’s immune responses. PD-L1 is a protein found in some types of cancer cells. When PD-1 attaches to PD-L1, it prevents T cells from destroying cancer. PD-1 and PD-L1 inhibitors prevent the PD-1 and PD-L1 proteins from attaching to each other. This allows T cells to fight the lymphoma. Immune therapy is suitable for effective treatment of recurrent Hodgkin’s lymphoma.
Radiation therapy is a non-invasive cancer treatment, in which high-energy X-rays or other types of radiation to kill abnormal cells or prevent them from growing are used. External beam radiation therapy involves the exposure of radiation to the area of the body where the cancer is found. Sometimes whole-body irradiation is given before a BMT procedure to slow down or stop the cancer process.

Radiation therapy is a non-invasive cancer treatment method that uses high-energy X-rays or other types of radiation to kill atypical cells or prevent them from growing. External beam radiation therapy involves applying radiation to the area of the body where the cancer is found. Sometimes whole body radiation is given before BMT to prepare the patient for the procedure.
External beam radiation therapy is effective for the treatment of Hodgkin’s lymphoma in adults, and can also be used as a palliative therapy to relieve symptoms and improve the quality of life of a patient with advanced lymphoma.
For a pregnant woman with Hodgkin’s lymphoma, radiation therapy should be delayed until delivery if possible. Risks should be avoided after exposure to radiation during fetal development. If treatment is needed immediately, the woman may decide to keep the pregnancy and undergo radiation therapy. A special lead shield is used to cover the belly of a pregnant patient in order to protect the fetus from radiation as much as possible.

In RIT, a monoclonal antibody is combined with radioactive material. When injected into the bloodstream, the radiation-bound monoclonal antibody travels to and binds to cancer cells, allowing a high dose of radiation to be delivered directly to the tumor.
Radioimmunotherapy in Israel is used to treat large B-cell lymphoma in patients who are newly diagnosed with the disease. RIT is also effective in cases where there is no response to chemotherapy treatment for different types of lymphoma.

The key parameters that affect how much the treatment of lymphoma in Israel costs are a set of therapy methods and a possible bone marrow transplant operation. For example, radiation therapy on the latest generation unit can cost up to $13,000 per course. Both autologous and allogeneic bone marrow transplantations are available to patients. BMT from a related donor for the treatment of lymphoma in Israel will cost approximately $174,000.
Up-to-date information on how much the treatment of lymphoma in Israel costs can be clarified at a free consultation with the coordinating doctor of Experts Medical.

- in Israel, children with lymphoma are admitted for treatment, which is not always possible in Western European countries;
- cost of BMT is less than in Germany and Spain with the same level of 5-year survival (about 95% according to clinics);
- no language barrier (staff often speaks English and Russian).
If you are looking for information about the quality of lymphoma treatment in Israel, reviews of clinics and doctors can be found on the Experts Medical website. To get personal advice from a company specialist, leave a request on this page. The doctor-coordinator will send your medical documents to the clinic and organize the treatment of lymphoma in Israel in a short time.













